
LEADING THE WAY IN CLINICAL AND HOSPITAL PBM THERAPY
The Australian Institute of Laser Therapy (AILT) was officially opened in the city of Melbourne on the 9th December 1997 by Secretary General of the World Association of Laser Therapy (WALT)


Dr Tiina Karu (left), renowned PhD researcher and cytobiologist in the field of photochemistry and photobiology, presented to Tina Czech the Director and senior technical consultant of the Australian Institute of Laser Therapy (AILT) with her latest autographed book; “Ten Lectures on the Basic Science of Laser Phototherapy”
Ms Tina Czech is the Director of the Australian Institute of Laser Therapy, who first became involved in photobiomodulation in 1990 when she met Dr Mary Dyson who was the head researcher at the Tissue Repair Research Unit at Guys’ Hospital in London.
At that time Mary and her research associates Peter Bolton and Stave Young were investigating the bio effects of laser light, in relation to the mechanisms which control the response of living tissue to injury and what influences laser light may have on healing processes and the quality of tissue repair.
Soon after Tina began integrating laser therapy into her clinical practice and for the next 7 years she utilised this modality for a wide range of soft and hard tissue injuries, post operative care, dermatological conditions, including burn injury, leg ulcers and amputations.
In 1997 Tina founded the Australian Institute of Laser Therapy as the first, government registered training organisation in Australia, for the dissemination of scientific information relating to laser and non-laser phototherapy and their clinical applications, which encompassed both laser photothermal activation and non-thermal photobiomodulation (PBM) and she was the founding President of the Australian Medical and Clinical Laser Association (AMCLA) that represented the AILT graduates.
Tina was invited to join the research team at the Royal District Nursing Service Helen Macpherson Smith Institute of Community Health, in Melbourne in 2008 as the educator and supervisor for PBM phototherapy in the first Australian Proof of Concept clinical study on the effects of low intensity laser therapy for relief of wound pain.
Ms Czech’s continuing dedication to the sharing of knowledge and her vast clinical experience has been instrumental in expanding the clinical application of laser PBM therapy into many areas of healthcare in Australia and her professional connections worldwide, continue to keep her up to date with the best technology available in photobiomodulation laser devices.
Tina now acts as a private consultant for the integration of PBM therapy and photomedicine into medical and hospital practice, as well as an advisor to new laser PBMT research projects.
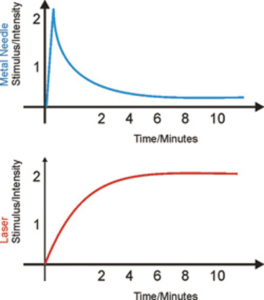
The photobiomodulating (PBM) effects of laser phototherapy, which was previously given the label of Low Level Laser Therapy (LLLT) involves transdermal application of light within the visible and near infra- red range of the electromagnetic spectrum using a laser or non-coherent light source. The primary effect begins intracellularly within the cell mitochondria, which is responsible for producing energy for the cell to function and regenerate new cells. While the secondary extracellular chemical reactions follow-on after the initial absorption of the light to support physiological and biological activity to assist in maintaining homeostasis that is essential to good health. These beneficial, light induced effects can continue for several hours or days after light exposure, which supports autologous healing, assists in reducing inflammation and pain and favourably improves neural and auto- immune function (Tuner J. Hode L. 2011., Karu, T. 1986,1988,1989a,1989b, 2012).
Research into photomodulated phenomena continued to be conducted worldwide in both in vitro and in vivo experiments and published in the first journal representing photobiomodulation research which was named ‘Laser Therapy’ and was the official journal for the International Laser Therapy Association (ILTA). Eventually in 1994 ILTA amalgamated with the International Society for Low Power Laser Applications in Medicine (ISLPLAM) and became the World Association for Laser Therapy (WALT) to represent this emerging field in phototherapy called low level or low intensity laser therapy (LLLT, LILT)), which was distinct from the photothermal activation by high level lasers used in surgery. As LLLT laser devices improved and effective treatment methodology continued to be developed, light-based technology expanded and so did the clinical applications of laser and non-laser light. Consequently, the term low level laser therapy was no longer applicable and the term PhotoBioModulation Therapy (PBMT) was agreed upon and with this progression the ‘Laser Therapy’ journal was renamed the journal for ‘Photobiomodulation, Photomedicine, and Laser Surgery’ and is now available in 170 countries.






Adam Canning is the Director of the ‘Wellness Clinic’ in Geelong, Victoria, who began his clinical career in 1997 at the Australian Institute of Laser Therapy. In 2009 he relocated to regional Victoria and established his well -known laser clinic in the Latrobe Health Centre.



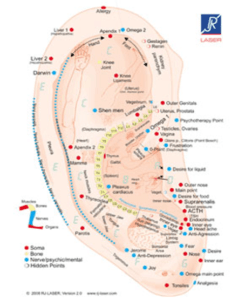
Over the past 25yrs Adam has been specialising in PBM therapy for sports medicine & tissue repair and pain management, as well as auriculotherapy for assisting in relieving chronic pain and neural disturbances associated to injury or trauma including PTSD, sleep disturbances, depression and anxiety and he liases with surgeons and medical practitioners in Geelong.
Adams previous background in homeopathy and auricular medicine brings a diverse approach to applying a combination of therapeutic modalities that provide positive, life changing outcomes for his clients, who have failed to fully respond to other types of treatment, and he is regularly invited to assist in our practical workshops and share his clinical experience and PBM treatment knowhow.
Dr Kerry Posniak (TCM) is a registered acupuncturist, laser therapist (LLLT) and Qigong facilitator and is the principal practitioner and founder of White Tiger Therapeutics clinic.
Kerry has also facilitated group acupuncture & Qigong classes at St Vincents Hospital in Melbourne as part of their detox program and was instrumental in developing the medical Qigong curriculum for the Chinese Medicine degree students at the Southern School of Natural Therapies, where she taught for 3 years.
With over a decade of clinical experience treating health related conditions, as well as fertility, anxiety, depression, addictions, digestive disturbances and chronic pain with herbal medicine, acupuncture and laser PBM therapy.
Kerry brings additional knowledge and expertise to the classroom and the practical component of our hands on Master courses.





Member: World Association for Laser Therapy (WALT)
Member: American Society for Photobiology (ASP)
Member: Wounds Australia
- About The Director
-
Ms Tina Czech is the Director of the Australian Institute of Laser Therapy, who first became involved in photobiomodulation in 1990 when she met Dr Mary Dyson who was the head researcher at the Tissue Repair Research Unit at Guys’ Hospital in London.
At that time Mary and her research associates Peter Bolton and Stave Young were investigating the bio effects of laser light, in relation to the mechanisms which control the response of living tissue to injury and what influences laser light may have on healing processes and the quality of tissue repair.
Soon after Tina began integrating laser therapy into her clinical practice and for the next 7 years she utilised this modality for a wide range of soft and hard tissue injuries, post operative care, dermatological conditions, including burn injury, leg ulcers and amputations.
In 1997 Tina founded the Australian Institute of Laser Therapy as the first, government registered training organisation in Australia, for the dissemination of scientific information relating to laser and non-laser phototherapy and their clinical applications, which encompassed both laser photothermal activation and non-thermal photobiomodulation (PBM) and she was the founding President of the Australian Medical and Clinical Laser Association (AMCLA) that represented the AILT graduates.
Tina was invited to join the research team at the Royal District Nursing Service Helen Macpherson Smith Institute of Community Health, in Melbourne in 2008 as the educator and supervisor for PBM phototherapy in the first Australian Proof of Concept clinical study on the effects of low intensity laser therapy for relief of wound pain.
Ms Czech’s continuing dedication to the sharing of knowledge and her vast clinical experience has been instrumental in expanding the clinical application of laser PBM therapy into many areas of healthcare in Australia and her professional connections worldwide, continue to keep her up to date with the best technology available in photobiomodulation laser devices.
Tina now acts as a private consultant for the integration of PBM therapy and photomedicine into medical and hospital practice, as well as an advisor to new laser PBMT research projects.
- What is PBM Therapy?
-
The photobiomodulating (PBM) effects of laser phototherapy, which was previously given the label of Low Level Laser Therapy (LLLT) involves transdermal application of light within the visible and near infra- red range of the electromagnetic spectrum using a laser or non-coherent light source. The primary effect begins intracellularly within the cell mitochondria, which is responsible for producing energy for the cell to function and regenerate new cells. While the secondary extracellular chemical reactions follow-on after the initial absorption of the light to support physiological and biological activity to assist in maintaining homeostasis that is essential to good health. These beneficial, light induced effects can continue for several hours or days after light exposure, which supports autologous healing, assists in reducing inflammation and pain and favourably improves neural and auto- immune function (Tuner J. Hode L. 2011., Karu, T. 1986,1988,1989a,1989b, 2012).
Research into photomodulated phenomena continued to be conducted worldwide in both in vitro and in vivo experiments and published in the first journal representing photobiomodulation research which was named ‘Laser Therapy’ and was the official journal for the International Laser Therapy Association (ILTA). Eventually in 1994 ILTA amalgamated with the International Society for Low Power Laser Applications in Medicine (ISLPLAM) and became the World Association for Laser Therapy (WALT) to represent this emerging field in phototherapy called low level or low intensity laser therapy (LLLT, LILT)), which was distinct from the photothermal activation by high level lasers used in surgery. As LLLT laser devices improved and effective treatment methodology continued to be developed, light-based technology expanded and so did the clinical applications of laser and non-laser light. Consequently, the term low level laser therapy was no longer applicable and the term PhotoBioModulation Therapy (PBMT) was agreed upon and with this progression the ‘Laser Therapy’ journal was renamed the journal for ‘Photobiomodulation, Photomedicine, and Laser Surgery’ and is now available in 170 countries.
- Our Team
-









Adam Canning is the Director of the ‘Wellness Clinic’ in Geelong, Victoria, who began his clinical career in 1997 at the Australian Institute of Laser Therapy. In 2009 he relocated to regional Victoria and established his well -known laser clinic in the Latrobe Health Centre.



Over the past 25yrs Adam has been specialising in PBM therapy for sports medicine & tissue repair and pain management, as well as auriculotherapy for assisting in relieving chronic pain and neural disturbances associated to injury or trauma including PTSD, sleep disturbances, depression and anxiety and he liases with surgeons and medical practitioners in Geelong.
Adams previous background in homeopathy and auricular medicine brings a diverse approach to applying a combination of therapeutic modalities that provide positive, life changing outcomes for his clients, who have failed to fully respond to other types of treatment, and he is regularly invited to assist in our practical workshops and share his clinical experience and PBM treatment knowhow.
Dr Kerry Posniak (TCM) is a registered acupuncturist, laser therapist (LLLT) and Qigong facilitator and is the principal practitioner and founder of White Tiger Therapeutics clinic.
Kerry has also facilitated group acupuncture & Qigong classes at St Vincents Hospital in Melbourne as part of their detox program and was instrumental in developing the medical Qigong curriculum for the Chinese Medicine degree students at the Southern School of Natural Therapies, where she taught for 3 years.
With over a decade of clinical experience treating health related conditions, as well as fertility, anxiety, depression, addictions, digestive disturbances and chronic pain with herbal medicine, acupuncture and laser PBM therapy.
Kerry brings additional knowledge and expertise to the classroom and the practical component of our hands on Master courses.






- Our Memberships
-
Member: World Association for Laser Therapy (WALT)
Member: American Society for Photobiology (ASP)
Member: Wounds Australia
Photobiology is an area of science that examines the chemical and physical changes induced by non-ionizing radiation and light in humans, plants, animals and micro-organisms, as well as the emission of light by biological systems. This involves the use of scientific tools to study the effects of different wavelengths on different molecules and the physical interactions of light with matter, including the vibration and rotation of molecules.
Photochemistry is a branch of chemistry that studies chemical reactions that occur due to absorption of light in the ultraviolet 100- 400nm, visible light 400-750nm and infra-red 750-2500nm part of the electromagnetic spectrum. Following absorption of a photon of light a chemical change can occur in the absorbing molecule e.g. Vitamin D synthesis in the skin after exposure to UV light.
Photobiomodulation instigates photochemical processes within humans and animals that can assist in restoring and maintaining homeokinetics and homeostasis within the biological system, following absorption of visible light and near infra- red wavelengths through the skin surface and this is known as PBM Therapy, previously called Low Level Laser Therapy LLLT.
- Photobiology
-
Photobiology is an area of science that examines the chemical and physical changes induced by non-ionizing radiation and light in humans, plants, animals and micro-organisms, as well as the emission of light by biological systems. This involves the use of scientific tools to study the effects of different wavelengths on different molecules and the physical interactions of light with matter, including the vibration and rotation of molecules.
- Photochemistry
-
Photochemistry is a branch of chemistry that studies chemical reactions that occur due to absorption of light in the ultraviolet 100- 400nm, visible light 400-750nm and infra-red 750-2500nm part of the electromagnetic spectrum. Following absorption of a photon of light a chemical change can occur in the absorbing molecule e.g. Vitamin D synthesis in the skin after exposure to UV light.
- Photobiomodulation
-
Photobiomodulation instigates photochemical processes within humans and animals that can assist in restoring and maintaining homeokinetics and homeostasis within the biological system, following absorption of visible light and near infra- red wavelengths through the skin surface and this is known as PBM Therapy, previously called Low Level Laser Therapy LLLT.
PRACTITIONER REVIEWS
I first integrated non-thermal, low level laser therapy, into my clinical practice with the RJ laser PBM equipment some 6 years ago and our clients were mainly sporting professionals and young recreational sports enthusiasts affected by physical trauma. Since then we have outgrown our clinic space and located to larger premises and continued to increase our range of RJ laser equipment because of it’s advanced German technology and ever increasing range of treatment options, in keeping with the latest scientific research in the field of photobiomodulation. Our scope of treatment has now expanded to include pre and post- operative therapy and rehabilitation, as well as, but not limited to; lumbago, sciatica, frozen shoulder, whiplash, chronic headache and neck pain, with an ever increasing focus on chronic pain and inflammation and in particular osteoarthritis and the advanced laser phototherapy education provided by the Australian Institute of Laser Therapy has been there right from the start and continues to provide that professional ongoing technical and clinical support.
As a Vet, I have always aimed to offer my animal patients the best care possible , but sometimes the healing process can be impaired by other factors.I have been implementing PBM Laser Therapy for the past 10 years using the RJ laser devices to enhance and accelerate the healing rate of all types of injury and neurological issues. There have been many times, when a severely injured and traumatised animal has been brought into my clinic and PBM therapy was applied to support the nervous system before we could do further investigations and necessary surgical procedures, but the survival of the animal was still in doubt. That is when daily applications of PBM therapy have aided the animal’s recovery and tissue regeneration beyond what we had originally expected, so we now apply PBM therapy as a standard procedure for all our animal patients.
I first integrated laser technology into the Coonabarabran Medical Centre back in 2005 after attending the Laser Induction course and hands-on practical training at the Australian Institute of Laser Therapy in Melbourne. Since then my nurses have also completed that same course, in order to assist me with the increase in patient demand for non- thermal laser PBM Therapy and this demand was largely due to patient word of mouth communication amongst our regional country community. Being in a north western NSW farming area, we have a high level of musculoskeletal complaints as well as injuries, coupled with acute and chronic pain, which we find PBMT highly effective for, as well as Diabetic leg ulcers and non -healing amputations and wounds and dermatological conditions. I utilise a variety of lasers from the RJ Laser range because of the diverse pre-programmed treatment menus, easy touch-screen operation and very fast treatment times that save me valuable time and effort in an already busy medical practice. I provide non-needle acupuncture, localised anatomical treatment and recently introduced non-invasive systemic PBM treatment, which we have found very beneficial for relieving anxiety and depression.
Our clinic is located on the state border towns of Albury & Wodonga. Darren has developed a thorough and holistic understanding of lasers and respects their innovative abilities to render optimum results for clients. We introduced this service to our Medical Aesthetic laser business in 2018, in which have now branched out as a separate business due to the success in this form of therapy. Darren has found using the RJ Laser for our PBM treatments to be non-invasive, pain-free, safe and effective for our patients.
Darren’s background in Nursing gives him a comprehensive understanding and respect for the importance of laser physiology to respect individual’s health, medical history and a high standard of care. Darren’s enthusiasm with lasers has seen him travel to Slovenia and Italy to help perfect the art of laser treatments for the clinic. In the course of Darren’s travels, he has created a network of professional contacts worldwide in the laser industry for professional support to help he is able to provide innovative, advanced and professional services to the wider community. Within our regional area we treat a broad range of musculoskeletal concerns, sporting injuries, post-operative healing, Endometriosis symptoms, mastitis treatment and dermatological conditions. We hope this modality gets more recognition as it deserves.
My focus as a naturopath is to support the body in restoring bioregulation and homeostasis and PBM therapy provides an efficient and safe mechanism for supporting the body’s natural healing processes. This form of laser therapy can be therapeutically beneficial during all phases of healing and recovery after illness, injury or surgery by alleviating pain and inflammation and supporting tissue regeneration and lymphatic drainage, naturally.
As a family doctor, I would be faced several times a day with patients who are suffering from chronic pain, which may not have been the main reason for their visits to me and I usually prescribed pain killers to provide temporary pain relief, knowing these may carry side-effects and do not address the underlying cause of the problem. Patients had often failed to get relief from other modes of physical therapy and I would feel helpless at not being able to offer definitive management of their pain stemming from injury or inflammation. After completing comprehensive and government approved training in laser photobiomodulation therapy (PBMT) and choosing what I considered to be the best laser equipment I could find from the Australian Institute of Laser Therapy, I began introducing this support therapy to some of my patients, who had very limited benefits from other clinical therapy modalities and a plethora of pain medications over the years. Initially I was surprised and delighted with the results and quickly began to accept that the speedy resolution of their symptoms, was not just a random effect, but a repeatable and effective one and without any unwanted side-effects. My clinical experiences since I introduced PBMT into my family medical practice has led me to believe that this modality is the way forward in managing chronic pain, pain medication addiction and associated mental health issues, just as it has proven to be in other countries around the world for the past 2 decades.
We have been using the RJ Laser equipment for many years now. The types of conditions we find the best results with in our patients have been neck pain, headaches, back pain (upper and lower), knee pain; and also the management of both acute and chronic injuries.
I purchased 2 lasers from the RJ Laser range for my hand therapy practice from the Australian Institute of Laser Therapy 18 months ago. Of all the modalities I have used in the past and currently still use, PBM therapy at this advanced level is by far the most versatile and effective management for a broad range of clinical applications, from acute trauma, post-operative management to chronic pain conditions. The analgesic and anti-inflammatory benefits are outstanding reducing the need for medication and in particular has offered a treatment option, for those slow to heal tendinopathies and ligament injuries and has accelerated healing timeframes. Tina Czech has been very responsive to our clinical queries and supporting us as we continue to successfully integrate PBM therapy into our routine rehabilitation.
Adding PBM to our Clinic has been of great value- Not only is it non invasive painless and comfortable, the effects of the therapy have provided a great support to our clients with a range of diverse problems including musculoskeletal, pain relief, aiding and accelerating recovery post surgery or post injury, reducing inflammation and oedema with lymphatic and autoimmune issues and overall assisting in the regeneration of all types of tissue.
We are loving the results and so are our clients!
Laser photobiomodulation has a unique place in treating many musculoskelatal conditions, including recurring pain in the shoulder, lower back, knee and foot without any manipulation of joints. I have found that laser is the best modality for improving healing response and pain relief in wounds and chronic leg ulcers and very quickly as well. My clients are amazed to see the scars almost disappear over a series of treatment sessions and in some cases nerve sensation returning to an area that had been numb for a long time.
At Roseville Wellness Group, Sydney, NSW we have found PBM to be very helpful for our patients. The many applications range from the usual musculoskeletal conditions (such as degenerative spine to acute trauma) to acupuncture approaches to healing and general wellbeing maintenance. We have found PBM is the only visibly effective treatment for lymphatic and G-lymphatic drainage. Good lymphatic and G-lymphatic flow as part of general wellbeing has become more prominent in clinical care today. Our PBM laser team (Jo, Tash, Deirdre and myself) have thoroughly enjoyed looking after the patients over the last two years and helping them achieve a better quality of life.
It may be time for clinical studies on PBM in patient care.
My pursuit of the best and most current knowledge in integrative Laser PBM Therapy(PBMT) and photomedicine as well as the most precise and potent laser systems available, led me to the Australian Institute of Laser Therapy (AILT) and Tina Czech who provided both. My personal experience with Induction and Masters level training with AILT opened a world of ground breaking multi-disciplinary practice with great possibilities and my interest to help a close family member with laser PBM therapy (PBMT) quickly expanded to my clinic patients, where results were promising and at the time, nothing short of incredible. I have been integrating laser PBMT and Osteopathic practice over the past 18 months using the RJ Physiolaser Olympic multiplatform PBM system and have been astounded by the treatment results so far. Not only have my ‘high’ expectations been breached, the possibility of greater heights for clinical success has been galvanised and made real by the treatment results I have obtained so far and would not have been possible without the support from Tina Czech and the highly experienced clinical consultants at AILT.












